Diabetes
NOUN
1. A disease in which the body’s ability to produce or respond to the hormone, insulin, is impaired, resulting in abnormal metabolism of carbohydrates and elevated levels of glucose in the blood and urine.
Diabetes affects your body’s ability to process sugar. Much of the food you eat is turned to sugar and used for energy. Normally, the pancreas releases insulin to help your body store and use the sugar and fat from the food you eat. Diabetes can occur when the pancreas produces very little or no insulin, or when the body does not respond appropriately to insulin. In Type I diabetes, the body doesn’t make enough insulin, a hormone that carries sugar from your blood to the cells that need it for energy. In Type II diabetes, the body stops responding to insulin altogether. Both case types result in high blood sugar levels, which can cause problems with your eyes, nerves, kidneys, heart and other parts of your body.
Currently, 29.1 million people living in the U.S. have diabetes. That’s 9.3% of the population. Approximately 1.7 million new cases are diagnosed each year—and 8.1 million people living with diabetes don’t even know they have it. As of yet, there is no cure, so people with diabetes need to actively manage their disease to stay healthy.
So what does this have to do with that smile of yours? What can you do about it? First, it’s important to understand the signs of diabetes and the roles they play in your mouth:
ORAL SYMPTOMS OF UNTREATED DIABETES
• You may have less saliva, causing your mouth to feel dry. (Dry mouth is also caused by certain medications.) You can fight this by drinking water regularly. You can also chew sugarless gum and eat healthy, crunchy foods to get saliva flowing. This is especially important because the sugar in your saliva, combined with less saliva available to wash away leftover food, puts you at a much higher risk of getting cavities.
• Gums may become inflamed and bleed often (gingivitis). If you notice some bleeding when you brush or floss, it may be an early sign of gum disease. If it becomes more severe, the bone that supports your teeth can break down, leading to tooth loss. Early gum disease can be reversed with proper brushing, flossing and diet Research has shown that gum disease can worsen if your blood sugar is not under control, so do your best to keep it in check.
• You may have problems tasting food. Your favorite flavors might not taste as good as they once did if you have diabetes. If this happens to you, take the opportunity to experiment with different tastes, textures and spices to your favorite foods. Just be careful not to add too much sugar to your food in an effort to add more flavor because not only does this affect the quality of your diet, it can also lead to more cavities. If you have a persistent bad taste in your mouth, see your dentist.
• You may experience delayed wound healing. Have you ever noticed a cold sore or a cut in your mouth that doesn’t quite seem to go away? This is yet another way diabetes can affect your mouth. Poor control of blood sugar can keep injuries from healing quickly and properly. If you have something in your mouth that you feel isn’t healing normally as it should, see your dentist.
o Implant success rates range from 92%-100% in patients with Type 1 diabetes and 94-100% in patients with Type 2 controlled diabetes.
o The average success rate for dental implants in non-diabetic patients is 97%-100%, so you can see that although there is a slightly higher failure rate for patients with diabetes, it’s not a staggering difference. The key is having the diabetes controlled prior to placing the implants.
• You may be susceptible to infections inside of your mouth. Diabetes also affects your immune system, leaving you more vulnerable to infection. One common problem experienced by people with diabetes is a yeast infection called oral thrush (candidiasis). The yeast thrive on the higher amount of sugar found in your saliva, and may look like a white layer coating your tongue and the insides of your cheeks. Thrush is more common in people who wear dentures and can often leave a bad taste in your mouth. See your dentist if you think you have thrush or any other mouth infection.
WHY ARE PEOPLE WITH DIABETES MORE PRONE TO GUM DISEASE?
Periodontal disease is the most common dental disease affecting people with diabetes, affecting nearly 22% of those diagnosed. Especially as we age, poor blood sugar control increases the risk for gum problems. People with diabetes are at a higher risk for gum problems because of poor blood sugar control. As with all infections, serious gum disease may also cause blood sugar to rise. This makes diabetes harder to control because you are more susceptible to infections and less able to fight the bacteria invading the gums.
HOW YOUR DENTIST CAN HELP
Regular dental visits are important. Research suggests that treating gum disease can help improve blood sugar control in patients living with diabetes, decreasing the progression of the disease. Practicing good oral hygiene and having professional deep cleanings done by your dentist can help to lower your HbA1c. (This is a lab test that shows your average level of blood sugar over the previous three months. It indicates how well you are controlling your diabetes.)
WHAT CAN YOU DO ABOUT IT?
Here are five oral health-related things you can do to for optimal wellness:
1 Control your blood sugar levels. Use your diabetes-related medications as directed, changing to a healthier diet and even exercising more can help. Maintaining a healthy blood sugar level will help your body fight any bacterial or fungal infections in your mouth and also help relieve dry mouth caused by diabetes.
2 Avoid smoking.
3 If you wear any type of a denture, be sure to clean it each day.
4 Brush your teeth twice a day with a SOFT toothbrush and clean between your teeth daily (with floss, water pik, or other interdental cleaning aids)
5 See your dentist for regular checkups.
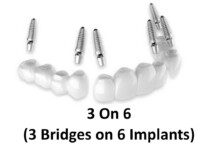
DENTAL IMPLANTS CAN HELP YOU MAINTAIN A HEALTHY DIET.
Have you noticed that the healthiest diets for diabetics include lots of fresh, whole foods that require extra chewing? The security and strength of dental implants makes it as easy and painless to eat the foods you want. Especially, when compared with dentures.
ARE DENTAL IMPLANTS SAFE FOR DIABETICS? Not only are dental implants safe for diabetics, forgoing dentures and opting for permanent dental implant supported teeth can improve the overall health for those with diabetes.
Not only do they help you comfortably maintain a well-balanced diet through better chewing ability, dental implants eliminate the inflammation and sore gums often associated with denture wear (or partial denture wear.)
Although patients with diabetes require special pre- and post-implant care, in order to minimize complications, recent studies show that dental implants are perfectly safe for those with controlled diabetes as long as their overall health complies with standard, pre-procedure health guidelines.
If you’re in need of dental care and have questions or concerns, CONTACT US to come see us for a complimentary consultation. We’re here Monday-Thursday. Call us today at 214-956-9100