1 of 42
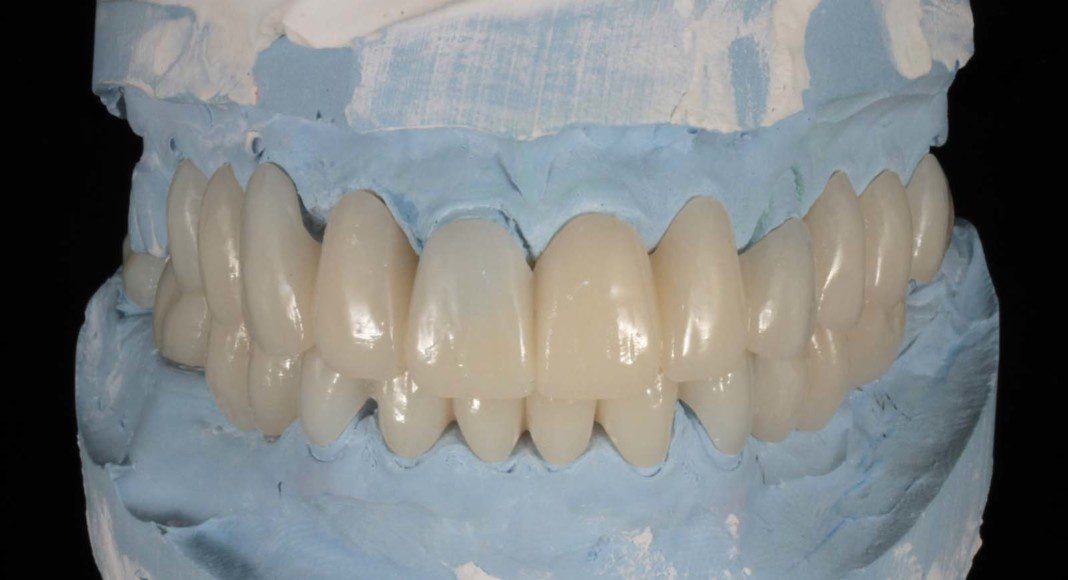
We start with a diagnostic wax-up and from that, these laboratory-processed provisional (temporary) acrylic (plastic) temporaries are fabricated.
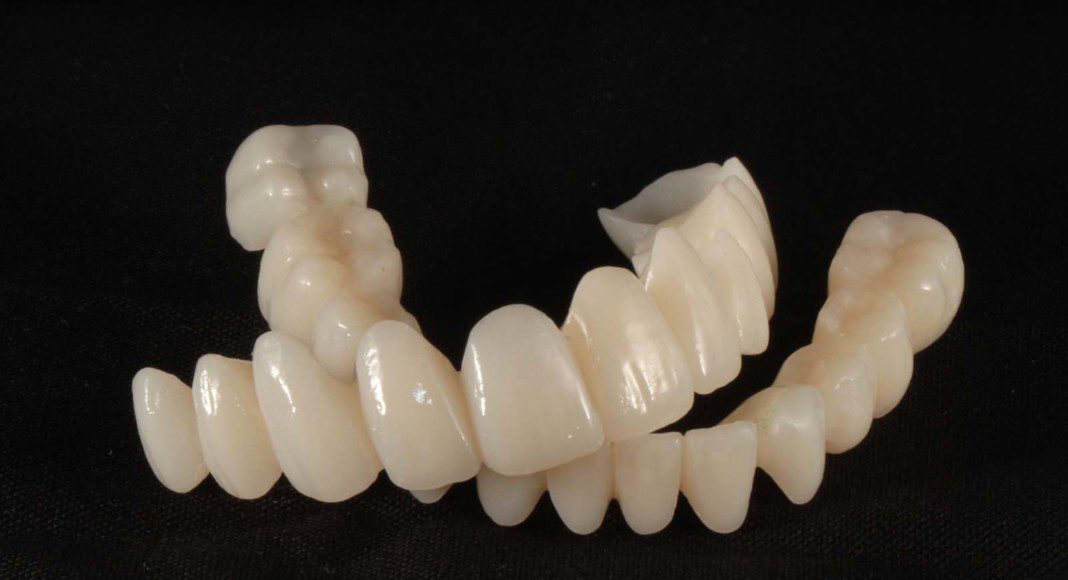
Temporary bridges off the stone model. We predict where the abutment teeth will be located at the surgery but we have latitude to modify these positions at the time of surgery.
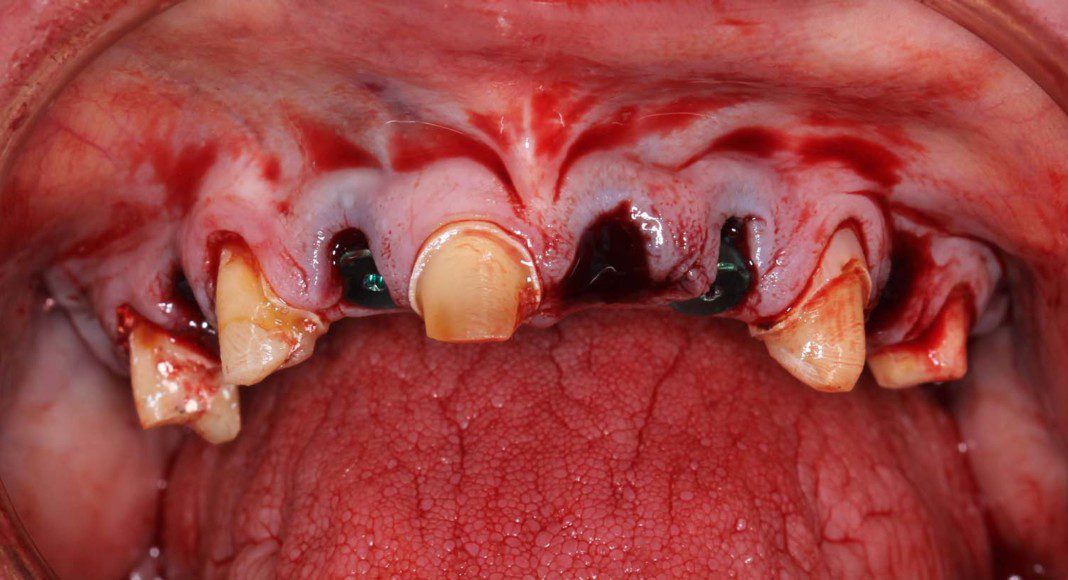
Stage one, upper, fixed temporaries on just teeth. Because not all the implants had adequate insertion torque (stability) we saved strategic teeth. These will serve as the interim abutments (supports) for the temporary bridge for two months. Transitional implant treatment does require a second surgery, more time and money but IT IS WORTH IT. Judge for yourself at the end.
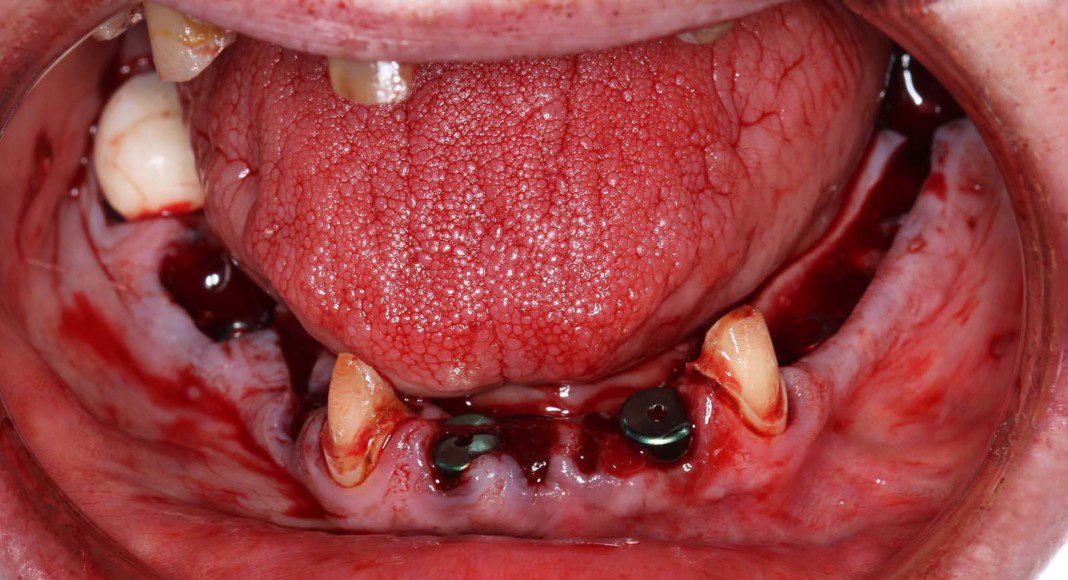
Lower bone is typically more dense than upper bone. In this case, we saved four teeth. When placing the implants there was adequate stability to support a fixed temporary. The teeth were extracted and the fixed temporary fabricated on the implants, only. If you’re a dentist viewing this case, DO NOT EXTRACT THE TEETH UNTIL YOU HAVE A TORQUE VALUE ON ALL IMPLANTS.
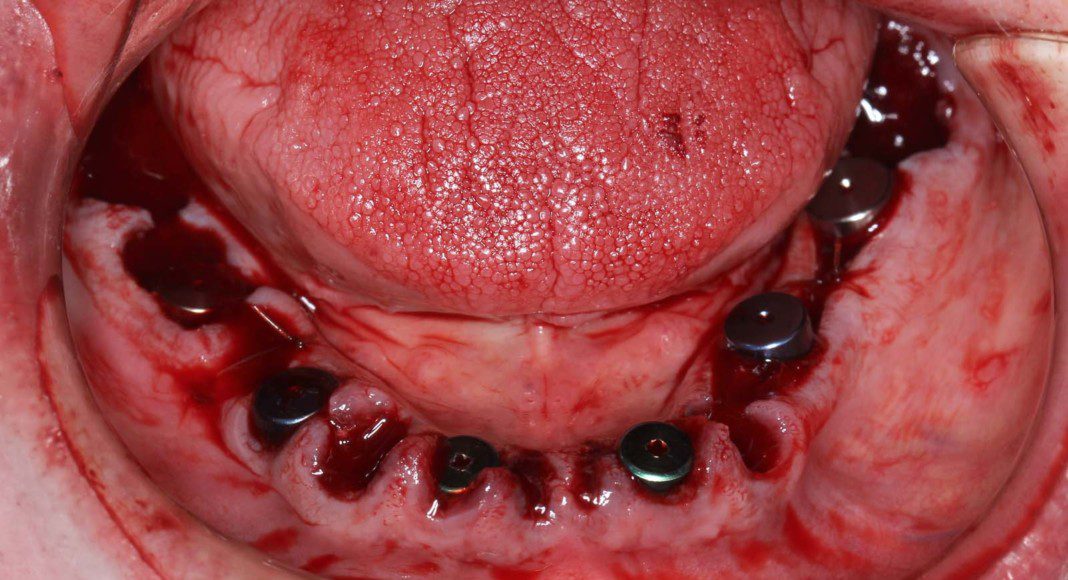
Once we determined that the implants all had adequate stability the remaining four teeth were extracted. Now, begins the fabrication of the temporary bridges.
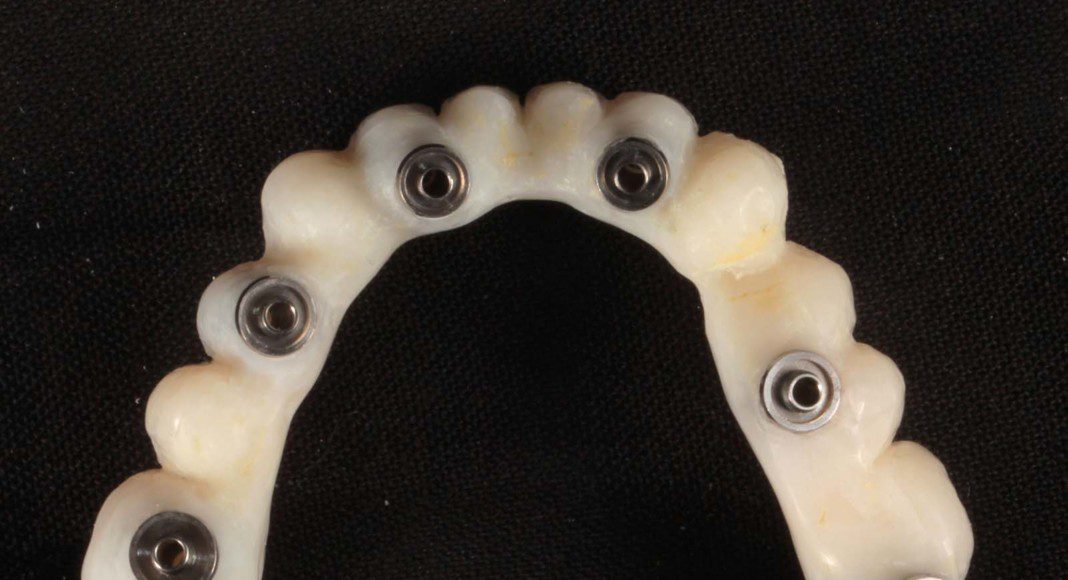
Same lower temporary showing the titanium cylinders where it directly connects the implants without abutments.
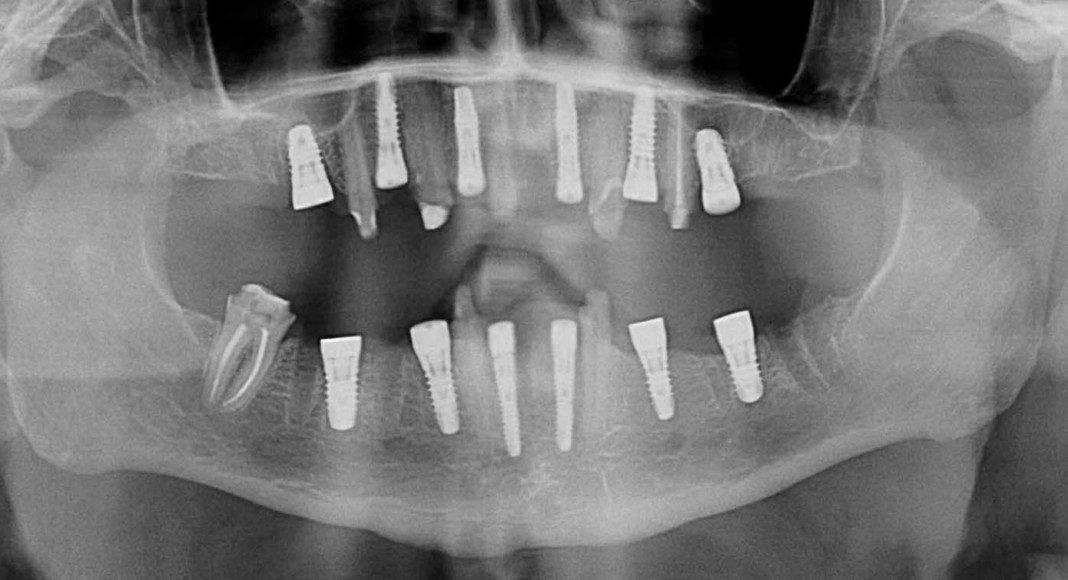
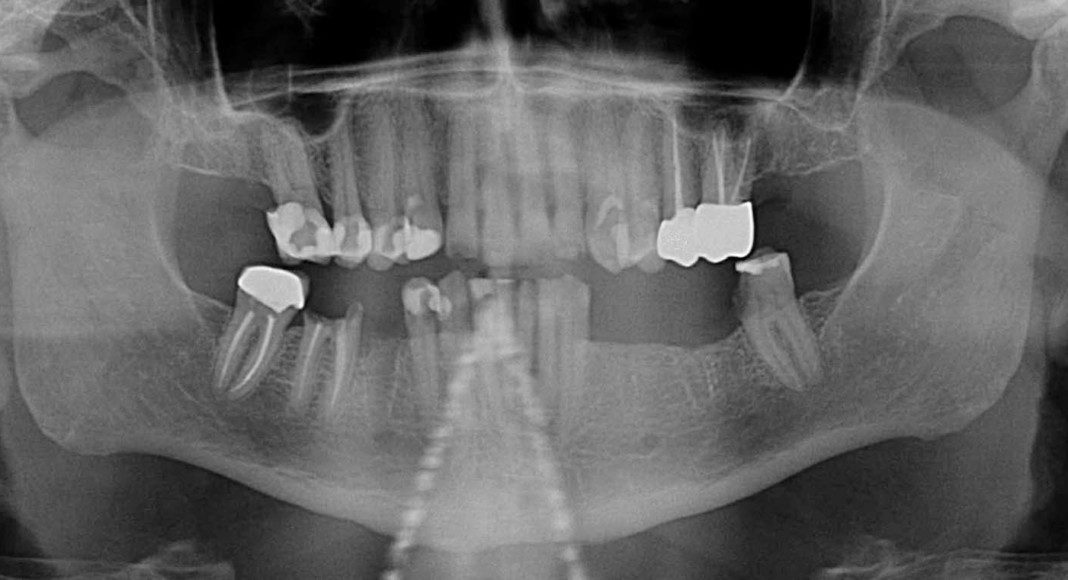
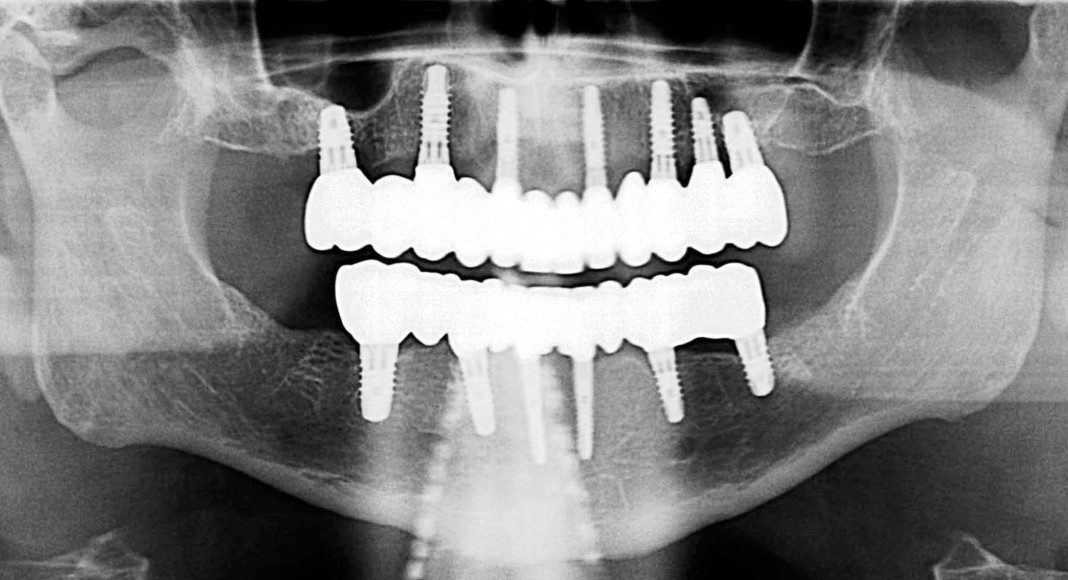
Progress panoramic x-ray. This x-ray really tells the story, visually. Notice the presence of teeth and implants. When immediate implant stability is not high enough to support the temporary bridge, we use some teeth as abutments (resting spots) for the temporary bridge. This prevents the patient from ever having to wear a temporary denture. This transitional phase allows the patient to be very comfortable while the implants are gaining stability (microscopic adhesion of the implant to the bone) and the temporary bridge is cemented to the strategic teeth.
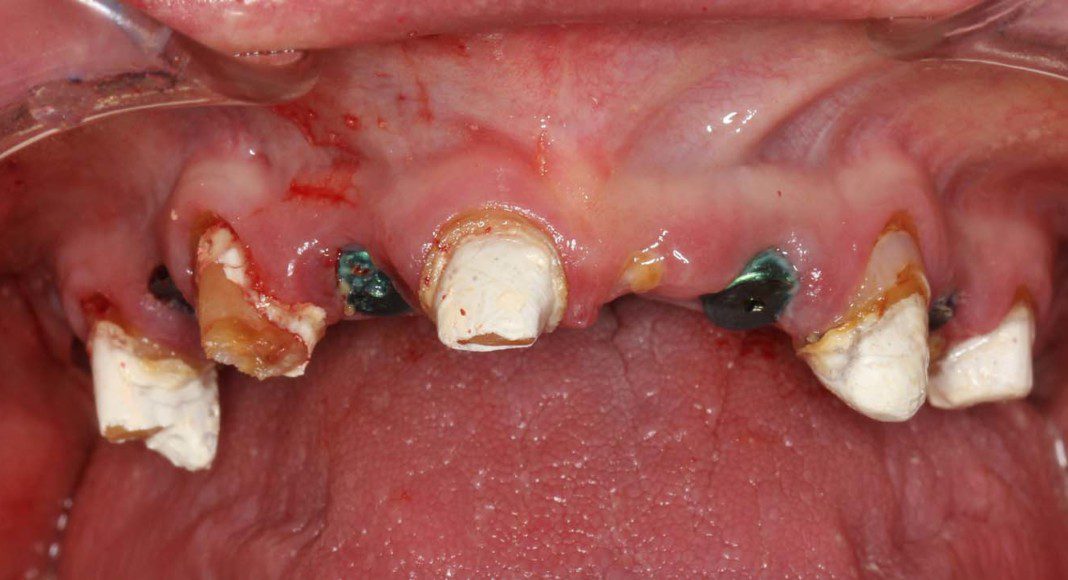
2 months later, teeth and implants after temporary is removed. The implants are now ready to serve as the anchors for the temporary bridge. At this second surgical appointment the strategic teeth are extracted, additional implants placed (if necessary) and the temporary bridge converted to the implants.
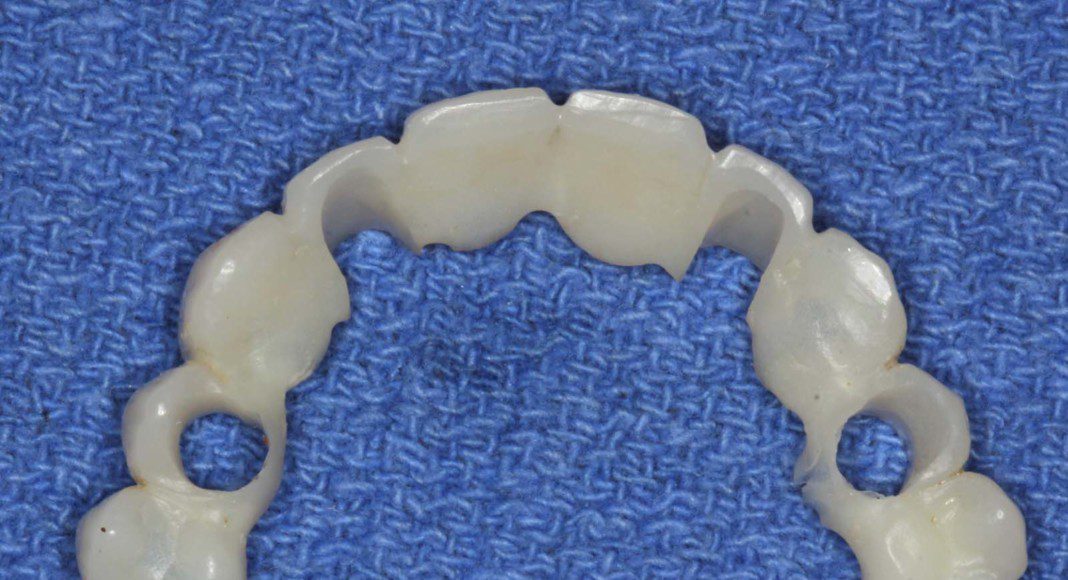
The previous temporary is modified to serve as the second temporary to be supported my implants, only.
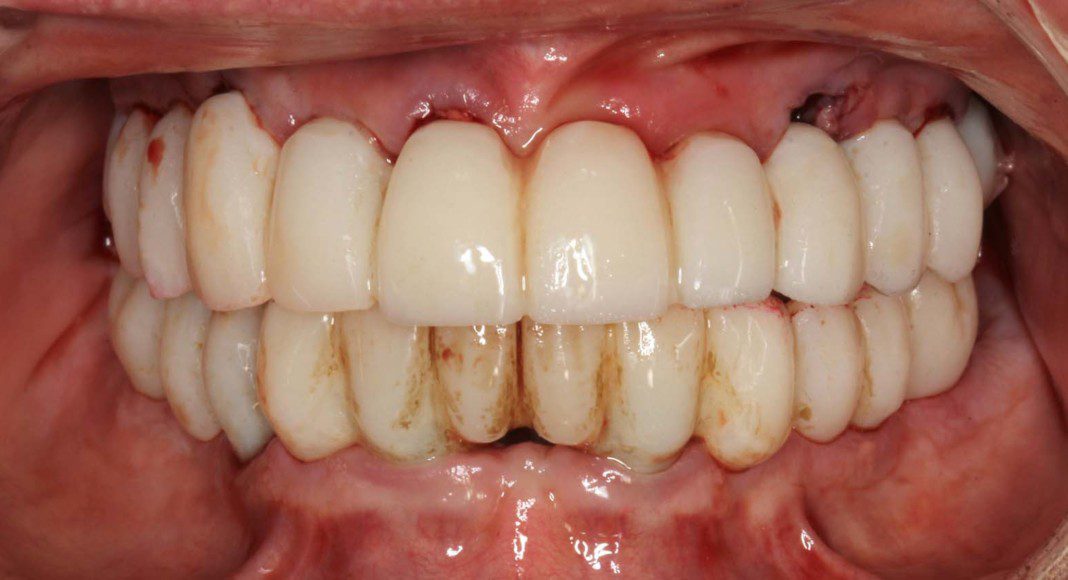
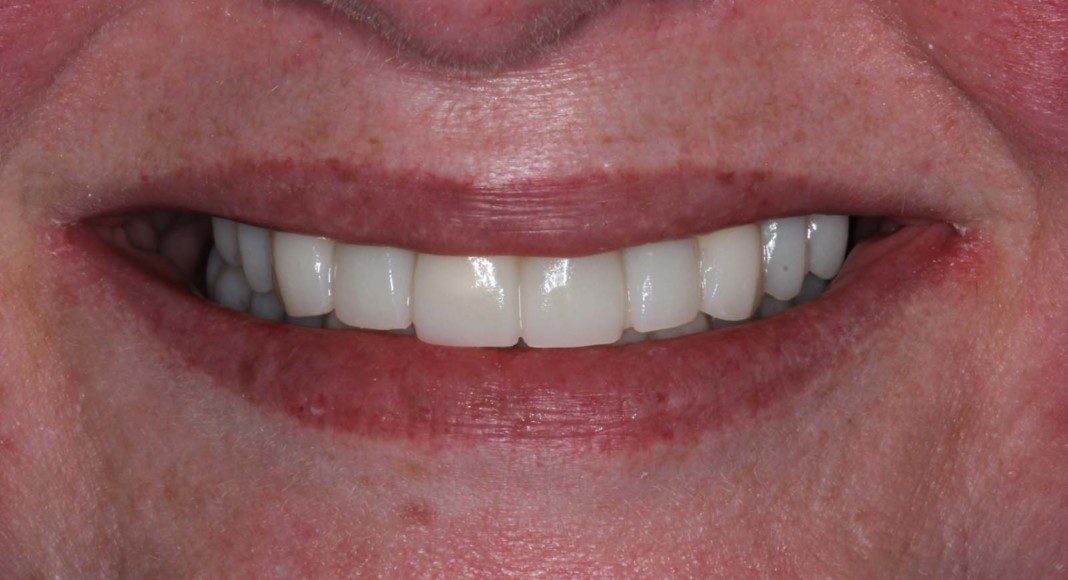
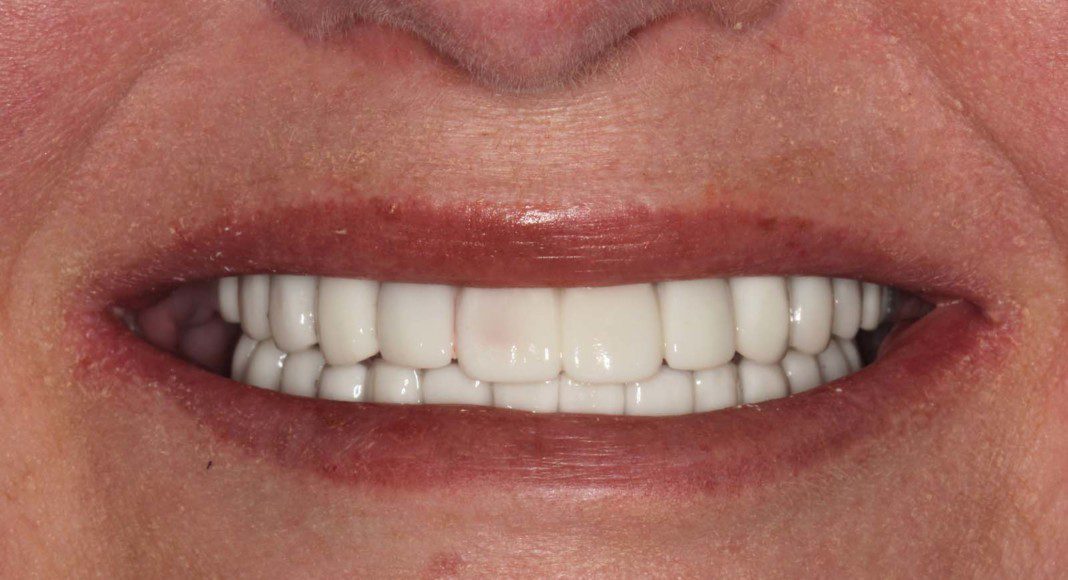
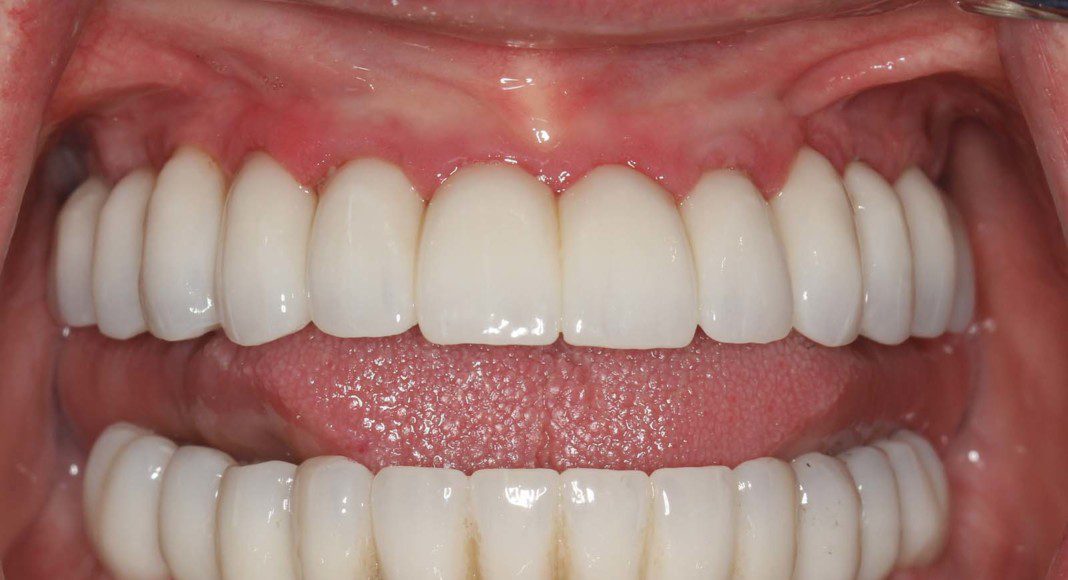
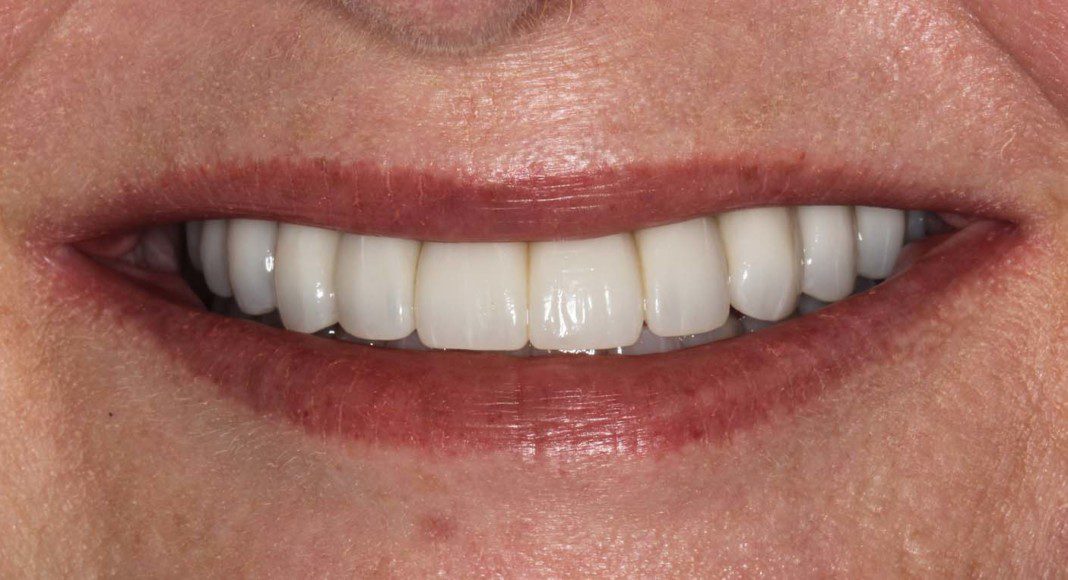
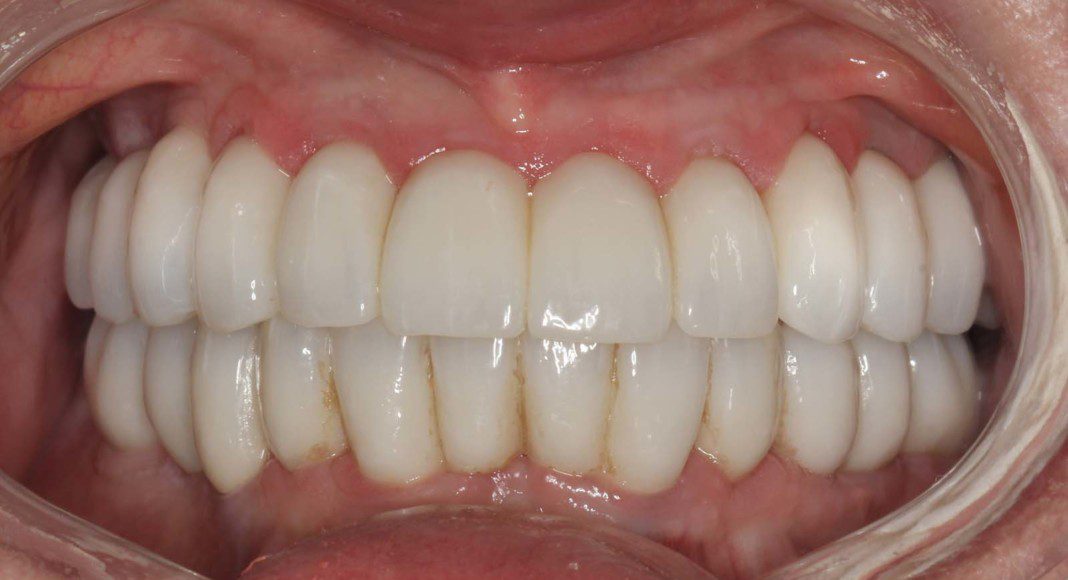
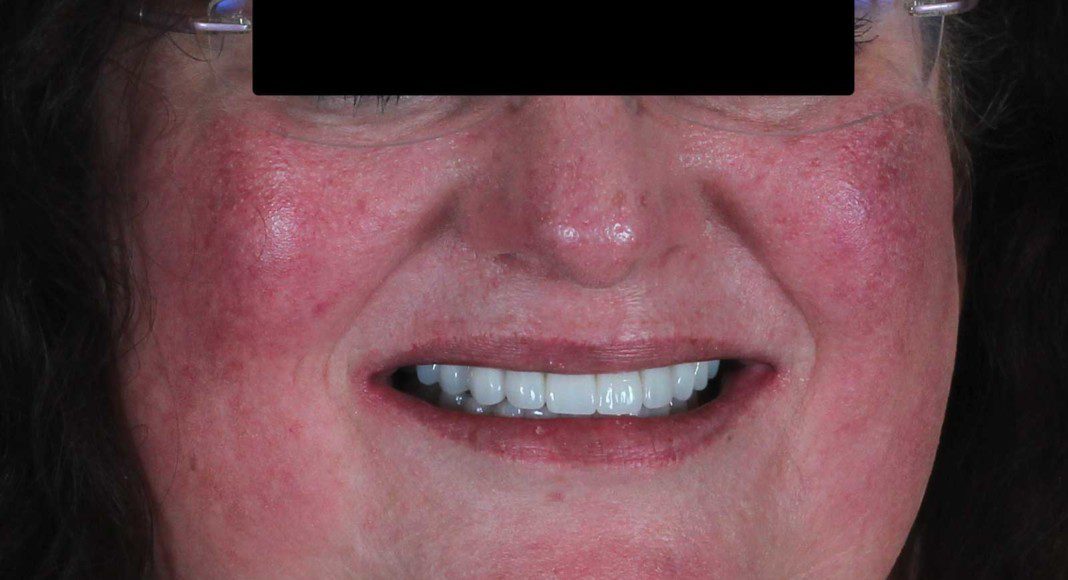
Frontal view of the implant temporary in the mouth. This temporary will stay in place for 2 more months as the bone and soft tissue remodel after the extractions.
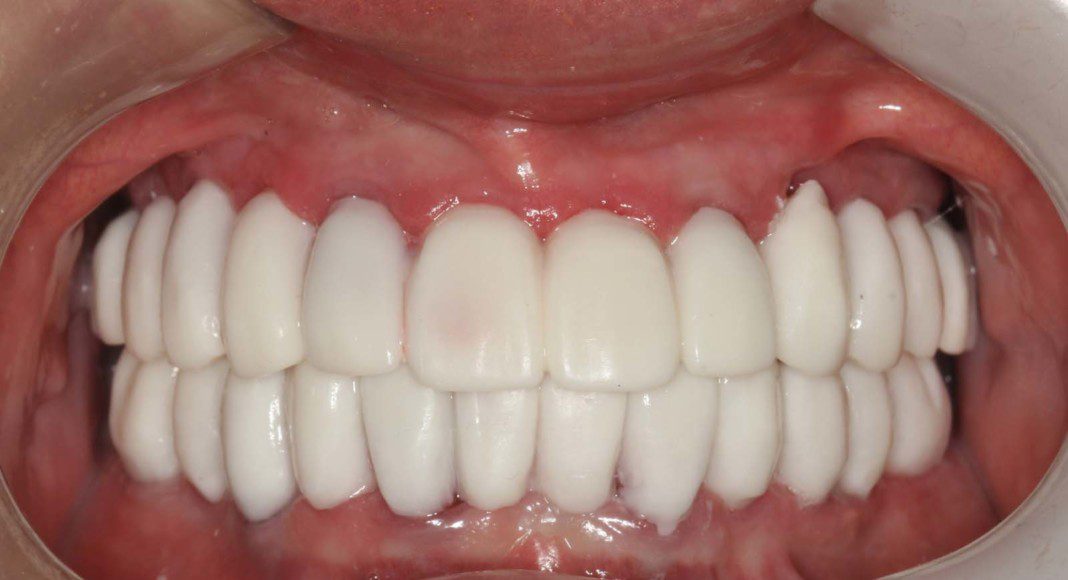
We are now ready to begin the fabrication process of the definitive, zirconia bridges. These are the wax protypes that we use to determine tooth length, width, proper bite (lip retracted). The patient and their family members are invited to this appointment so that everyone can view the over aesthetics before we process in zirconia. Once it’s in zirconia, we cannot make big changes.
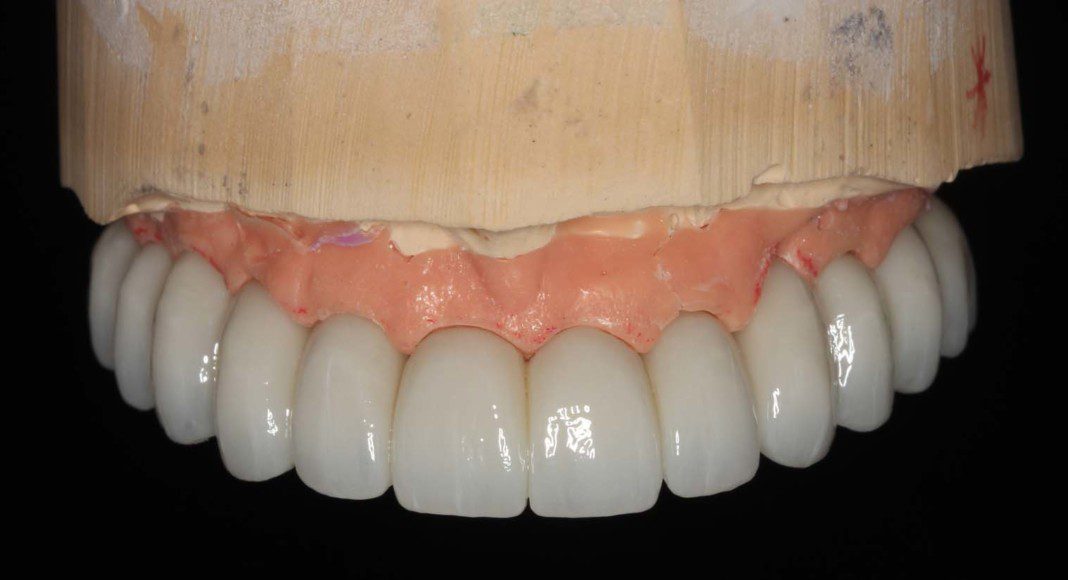
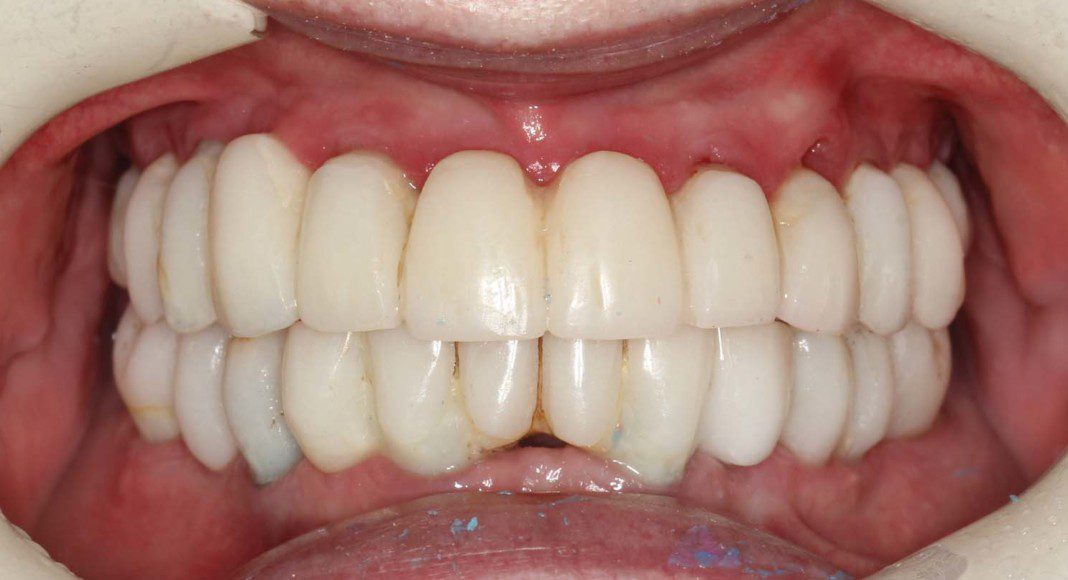
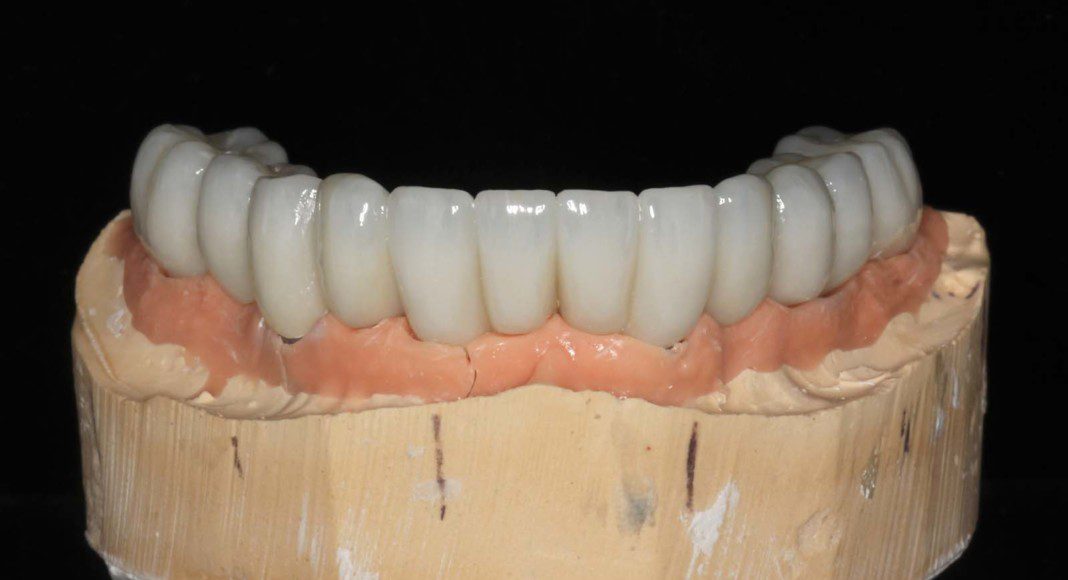
Once everyone is satisfied, we can send the wax-up to the lab for scanning, milling and customization. Here is the upper, zirconia bridge on the master cast (frontal view).
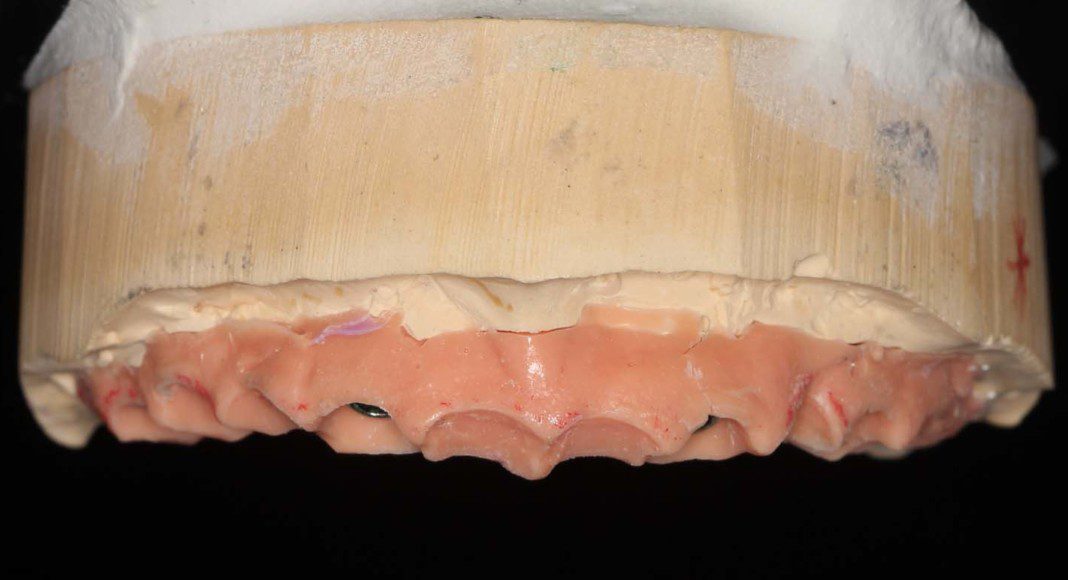
Frontal view, master cast with tissue moulage (simulated gum tissue). Because this material can be modified, we modify it to guide the tissue contours beyond what we did in with the temporary bridges.
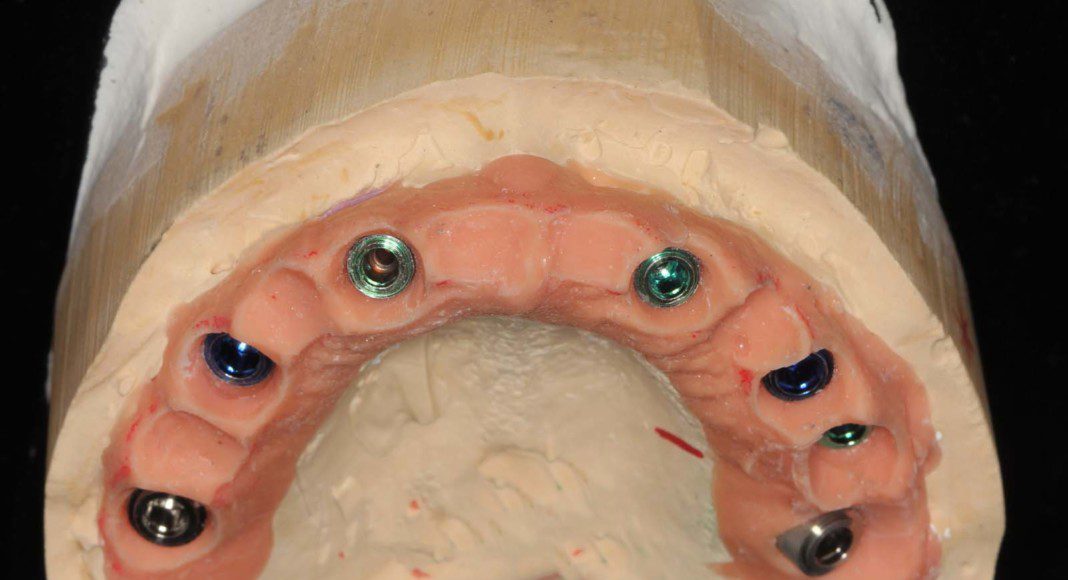
Occlusal view, master cast with tissue moulage (simulated gum tissue). Because this material can be modified, we modify it to guide the tissue contours beyond what we did in with the temporary bridges.
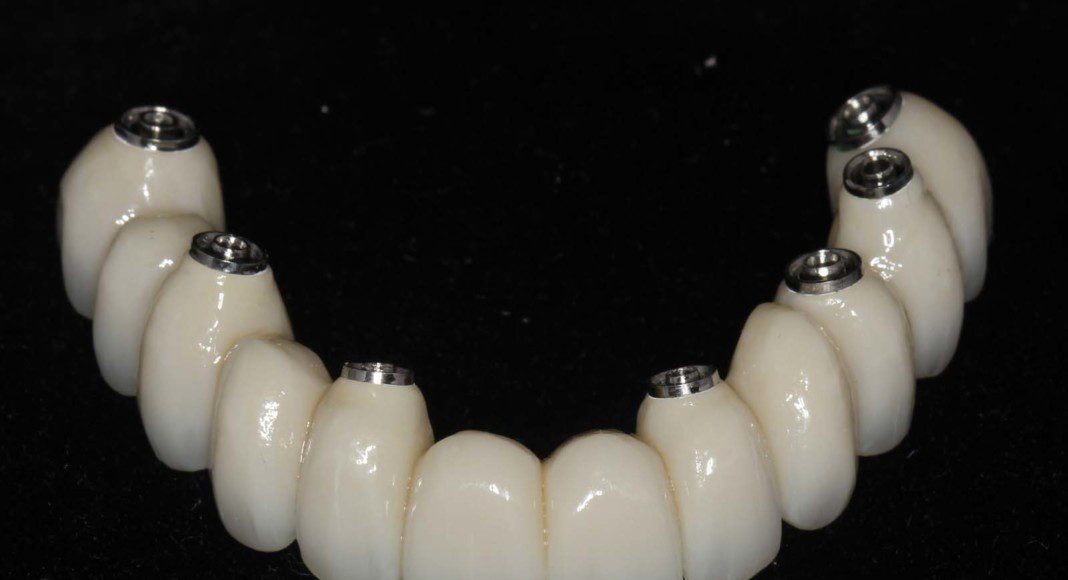
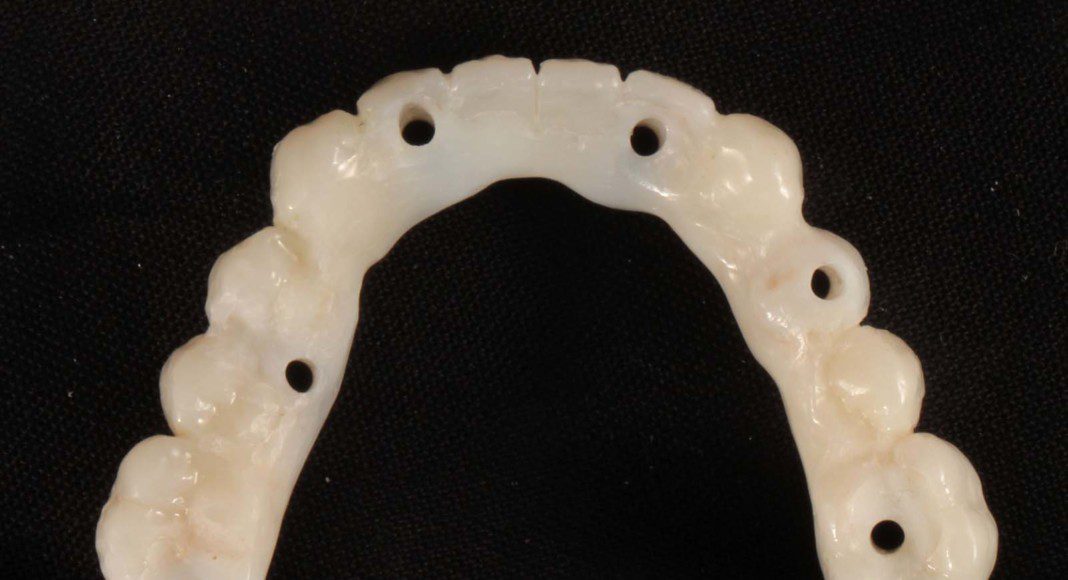
The intaglio (tissue side) of the upper, zirconia bridge. The contours are “convex” not concave for easy hygiene.
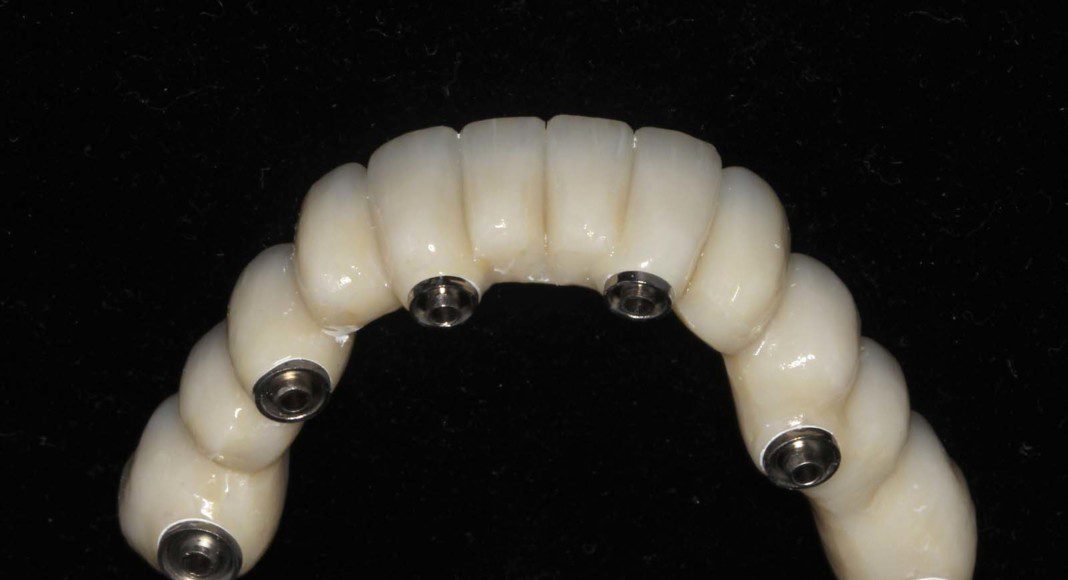
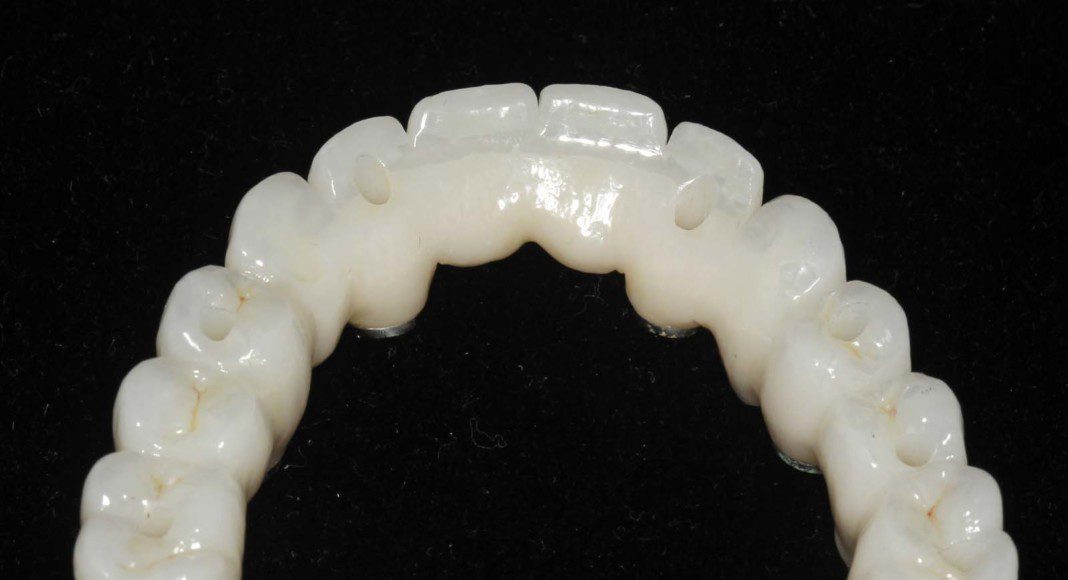
The intaglio (tissue side) of the lower, zirconia bridge. The contours are “convex” not concave for easy hygiene.
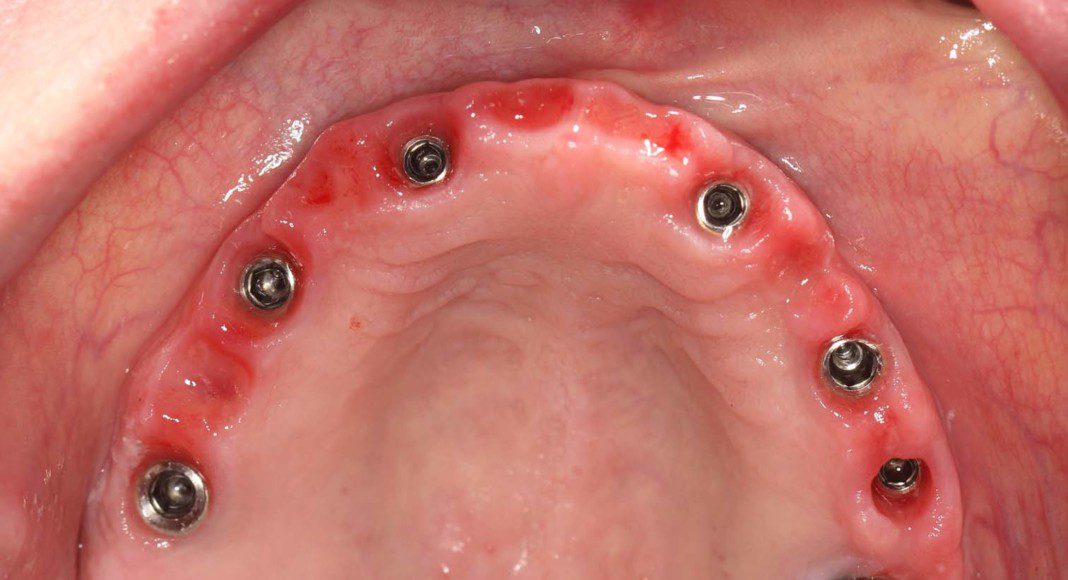
Occlusal view of the upper arch. Note: The tissues are a little red. Many patients, especially women have a slight allergy to the acrylic of the temporary bridges. This resolves after the zirconia bridge is placed.
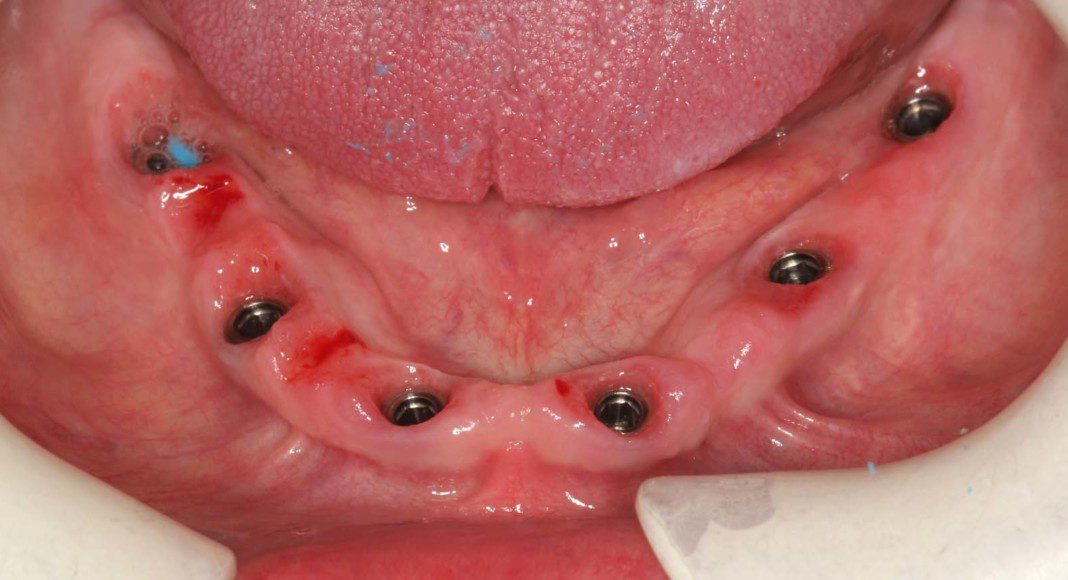
Occlusal view of the lower arch. Note: The tissues are a little red. Many patients, especially women have a slight allergy to the acrylic of the temporary bridges. This resolves after the zirconia bridge is placed.
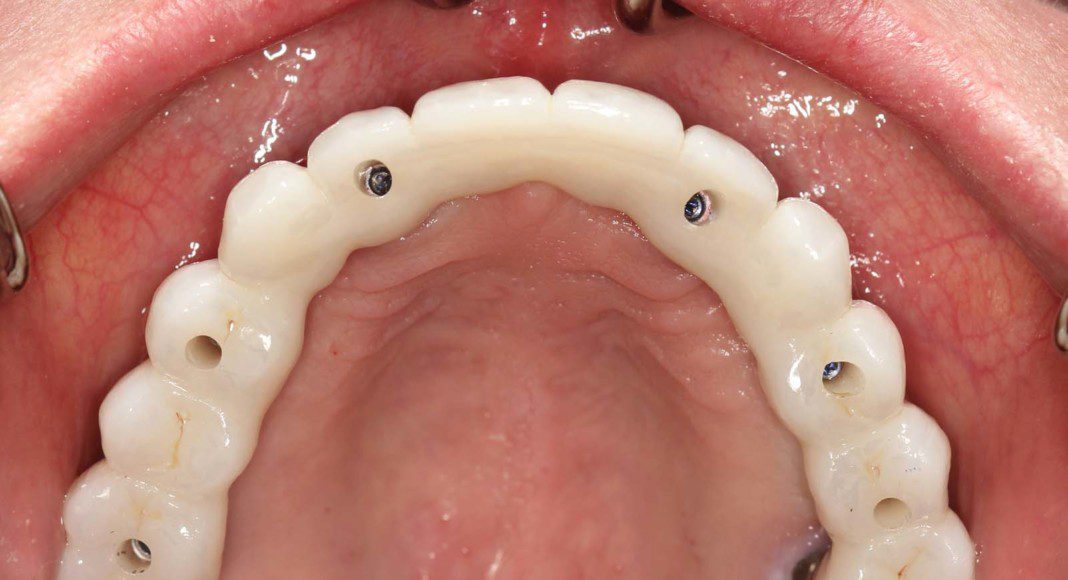
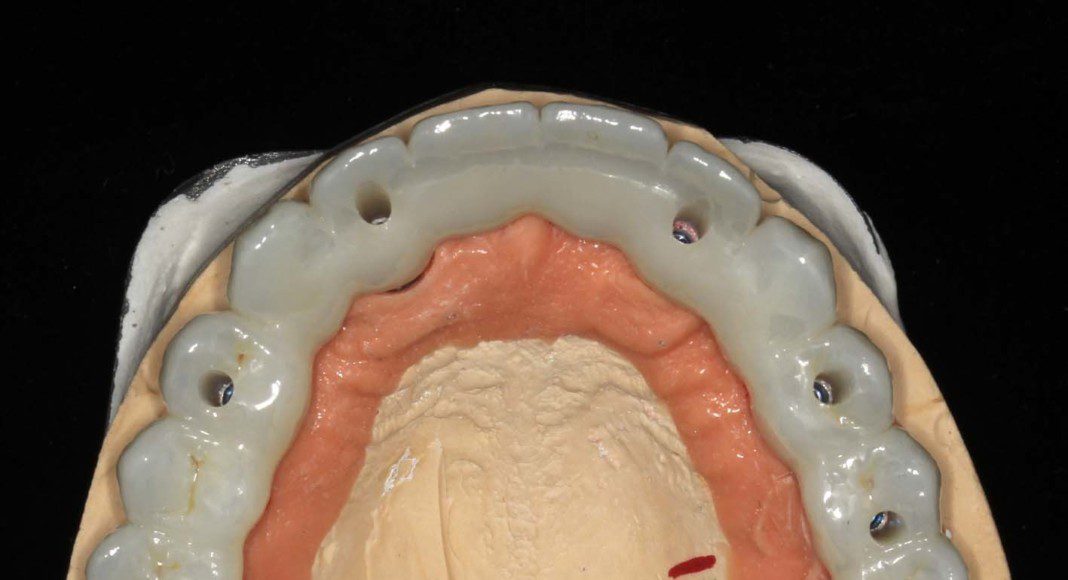
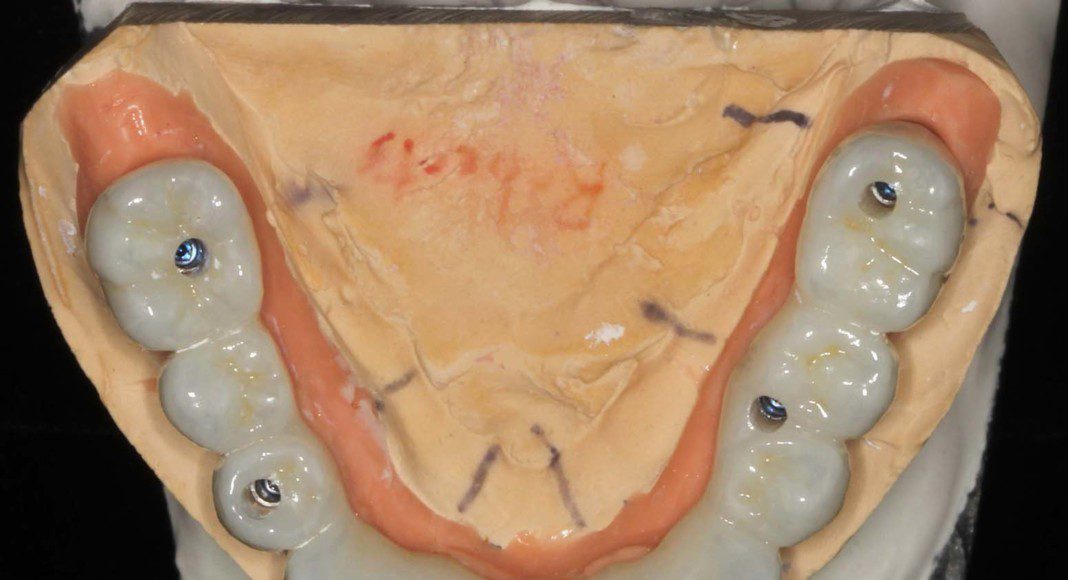
Occlusal view, upper, day of delivery. If you look closely, you can see the final prosthetic screw (blue). This channel is covered with composite resin.